Introduction
Nobody warned you about this one. The pregnancy books covered heartburn and swollen ankles. The forums were full of morning sickness stories. But nobody talked about that breathtaking, sharp pain that seizes you the moment you roll over in bed, swing your legs out of the car, or stand on one foot to pull on your socks.
What you are experiencing has a name: sacroiliac (SI) joint pain. It is the single leading cause of pregnancy-related back and pelvic pain, it affects close to half of all pregnant women, and yet it is one of the least talked-about discomforts in prenatal care. Most first-time moms spend weeks not knowing what is happening in their bodies only that moving suddenly hurts in a very specific, very startling way.
This guide is going to change that. By the time you finish reading, you will know exactly what your SI joint is, why pregnancy affects it so dramatically, how to tell it apart from other conditions like sciatica, and most importantly what you can do right now to feel better without waiting for an appointment or the end of your pregnancy.
What Is the SI Joint and Why Does It Matter?
Your sacroiliac joints sit exactly where the two large bones of your pelvis called the iliac bones connect to the triangular bone at the base of your spine, called the sacrum. You have one on your left and one on your right, tucked right behind those two small dimples at the very bottom of your back. Press your thumbs there and you have found them.
In ordinary life, the SI joints are built for stability above almost everything else. They are anchored by some of the thickest, toughest ligaments in the entire human body, and they move only about two to four millimeters in any direction under normal conditions. Their primary function is elegant and essential: they transfer the weight of your entire upper body down into your legs with every step, and they absorb the upward shock from the ground before it reaches your spine. They are, effectively, your body’s central shock-absorbing hinge.
Because these joints are designed for strength and stability rather than for wide-range movement, they can become acutely painful when that stability is disrupted. And pregnancy disrupts it in several simultaneous ways which is why SI joint pain is so common, and why it can appear or worsen quickly as your body changes.
How Common Is SI Joint Pain During Pregnancy?

50% of all pregnant women experience pelvic girdle pain, with the SI joint identified as the primary source in most cases
95%+ of pregnancy-related leg and back pain traces back to the SI joint not the sciatic nerve, as is commonly assumed
26% of women still have unreported SI joint pain after delivery, often mistaking it for normal postpartum recovery soreness
Considering how many women are affected, it is striking how rarely SI joint pain gets named or explained in prenatal appointments. Many women walk around for weeks thinking they have a pulled muscle, general back pain, or sciatica all while doing nothing that specifically helps their actual problem. Understanding what is happening is the first step toward genuine relief.
Who Is at Higher Risk?
SI joint pain can develop in any pregnant woman, but certain factors make it significantly more likely and more persistent. Knowing your risk profile helps you start protecting yourself earlier.
Pre-existing back or pelvic pain
Women who experienced lower back pain or pelvic discomfort before becoming pregnant are at considerably higher risk during pregnancy.
Weak glute and core muscles
The muscles that protect the pelvis especially the glute medius are the body’s first line of defense. Weakness here leaves the SI joint exposed.
Previous pelvic injury
A history of falls, car accidents, or sports injuries affecting the pelvis or tailbone increases joint vulnerability during pregnancy.
Carrying multiples
Twin or triplet pregnancies place far greater mechanical and hormonal stress on the pelvis, escalating SI joint risk significantly.
Pain that starts before 20 weeks
Early-onset SI joint pain is associated with more persistent symptoms throughout pregnancy and a greater risk of pain continuing well into the postpartum period.
Breastfeeding
Nursing keeps relaxin the hormone that loosens pelvic ligaments elevated in the body, which can delay natural joint restabilization after birth.
Four Reasons Your SI Joint Hurts During Pregnancy
SI joint pain during pregnancy is not caused by one thing going wrong. It is the result of several changes converging on the same joint at the same time. Understanding each cause is useful because each one also represents an opportunity to intervene.
1: Relaxin A Necessary Hormone With an Uncomfortable Side Effect
Shortly after conception, your body begins producing a hormone called relaxin. Its purpose is purposeful: it gradually loosens the ligaments around your pelvis so that your body can eventually open enough during labor to allow your baby through. However, the same ligament loosening that prepares you for birth also reduces the natural stability your SI joints depend on daily. With less tension holding them in place, the joints can move slightly more than they should and that excess movement triggers inflammation, irritation, and pain. Research now confirms that relaxin alone does not tell the whole story; it creates the conditions for pain, but other factors determine whether pain actually develops and how severe it becomes.
2: Shifting Center of Gravity and Changing Posture
As your baby grows, your center of gravity moves forward and downward. To stay balanced, your lower back arches more deeply than usual a postural shift called increased lumbar lordosis and your pelvis tilts forward in response. This new alignment places sustained mechanical stress on the SI joints in ways they were not built to handle for extended periods. At the same time, your feet naturally rotate outward to widen your base of support (the medically recognized “pregnancy waddle”), which shortens your hip muscles and reduces their effectiveness as shock absorbers pushing even more load directly onto the joint itself.
3: Weakened Abdominal and Core Muscles
As your uterus expands, your abdominal muscles including the rectus abdominis and the internal and external obliques stretch and thin considerably. Research measuring muscle changes in pregnant versus non-pregnant women has confirmed that these muscles weaken meaningfully as the pregnancy progresses. Since your core muscles form part of the same stability system that protects your pelvis and spine, losing their contribution means your SI joints must absorb forces alone that they were never meant to handle without muscular backup. A joint that is simultaneously more mobile (due to relaxin) and less protected (due to core weakness) is one that will reliably hurt.
4: Asymmetric Joint Laxity The Reason One Side Hurts More
Here is a cause that most articles skip entirely. Not all SI joint loosening in pregnancy is equal on both sides. Peer-reviewed research has found that women whose left and right SI joints loosen unevenly a condition called asymmetric sacroiliac joint laxity have up to three times the risk of developing moderate to severe pelvic girdle pain compared to women with balanced laxity. This explains why so many women feel pain predominantly on one side, why the painful side sometimes changes, and why generic advice does not always work for everyone. The underlying asymmetry requires specific assessment and targeted treatment to address properly.
How SI Joint Pain Changes Through Each Trimester
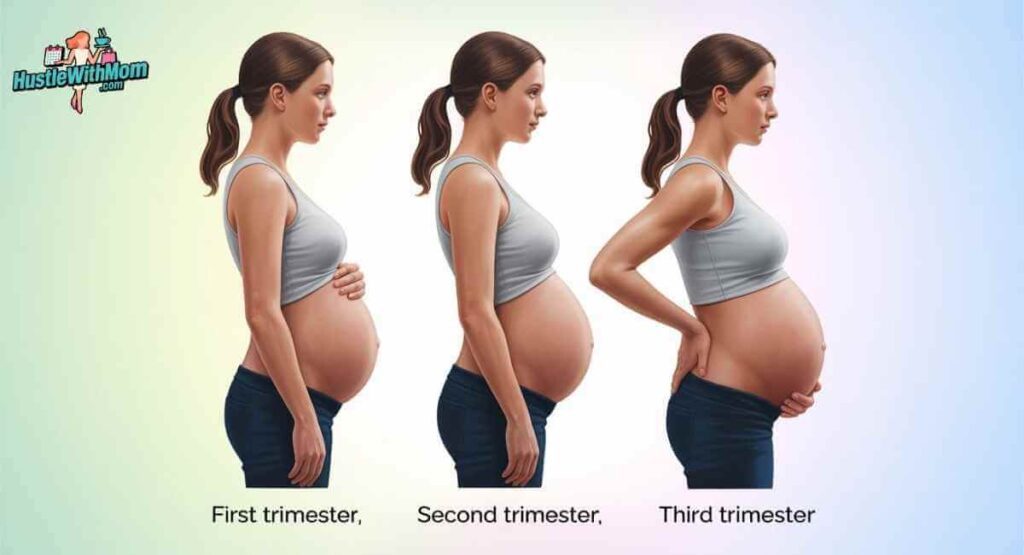
SI joint pain rarely feels the same from the first week to the last. Recognizing how it typically progresses can help you identify it earlier and respond before it becomes severe or debilitating.
First Trimester · Weeks 1 to 12
Early Sensitivity That Many Women Miss
Relaxin rises quickly after conception and peaks during the first trimester. Some women notice subtle aching or instability in the lower back or hips as early as weeks six to ten. Many dismiss this as general pregnancy tiredness or growing pains and never connect it to the SI joint. However, pain that begins before 20 weeks is a signal worth reporting to your healthcare provider, as early-onset symptoms are associated with a more persistent course later in pregnancy and postpartum.
Second Trimester · Weeks 13 to 26
The Window When Most Women First Notice It
The majority of first-time moms with SI joint pain first experience it clearly between weeks 18 and 24. The baby is growing quickly, abdominal muscle support is diminishing, and postural compensation is accelerating. This is typically when women describe that sudden, gasping pain when rolling over in bed or stepping out of the car the pain that feels like it came from nowhere. Addressed at this stage, it is highly treatable. Ignored, it tends to worsen through the third trimester.
Third Trimester · Weeks 27 to 40
Peak Demand on the Pelvis
The third trimester places the greatest physical demand on your SI joints. The baby’s weight is at its highest, your posture has changed substantially, your core muscles are at their most stretched, and ligament laxity is near its maximum. Pain during this phase often becomes more constant, affecting sleep, walking pace, and the ability to perform basic tasks. This is when a maternity support belt tends to be most immediately helpful, and when consistency with strengthening exercises pays off most clearly.
Labor and Delivery
An Added Stressor Worth Preparing For
Birth itself can strain the SI joints further particularly during prolonged labor, with certain delivery positions, or if instrumental assistance is used. Women who enter labor with pre-existing SI joint dysfunction tend to have more significant postpartum pain. Working with a pelvic health physical therapist during pregnancy gives you both a stronger pelvis for labor and better tools for recovery once your baby arrives.
Recognizing SI Joint Pain: What Does It Actually Feel Like?
SI joint pain has a recognizable character, though the intensity varies widely from woman to woman. The defining feature is this: the pain is almost always triggered or worsened by specific movements particularly any activity that loads just one side of your pelvis at a time, even briefly.
One-Sided Lower Back Pain
Sharp or aching pain right at the dimple above your buttock usually on one side, though it can occasionally shift or affect both sides.
Pain Into the Buttock or Upper Thigh
Pain that travels into the buttock, groin, or back of the upper thigh. Crucially, it rarely travels past the knee.
Rolling Over in Bed
The most commonly reported trigger: a sharp, startling pain when turning over during the night or lifting yourself out of bed in the morning.
Getting In and Out of the Car
The pivoting and leg-swinging motion of exiting a vehicle places a rotational force on the SI joint that is a very reliable flare trigger.
Dressing While Standing
Standing on one leg for even a few seconds to put on socks, shoes, or trousers is one of the fastest ways to produce sudden SI joint pain.
Climbing Stairs
Each step requires loading one leg fully while the other lifts, creating the asymmetric pelvic force that aggravates the SI joint most.
Clicking or Catching Sensation
Some women feel or hear a click, pop, or catching sensation in the hip or pelvic area when walking, turning, or changing positions.
Significant Morning Stiffness
A stiff, painful feeling in the lower back, hips, and buttocks upon waking which often eases gradually with gentle movement over the first 20 to 30 minutes of the day.
📌 A Helpful Pattern to Notice
If you can find a position such as lying on your back with your knees bent and supported that gives you noticeable relief from your pain, that is a strong indicator the pain is musculoskeletal in origin and likely related to the SI joint. Pain that responds to position changes almost always has a mechanical cause. Pain that feels identical regardless of what you do warrants prompt medical attention.
SI Joint Pain vs. Sciatica During Pregnancy How to Tell Them Apart
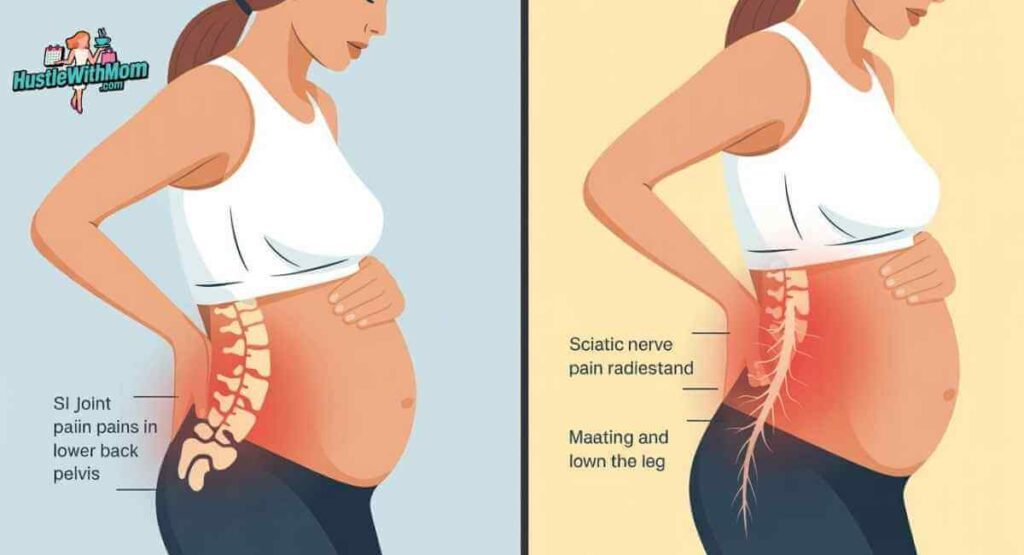
This distinction matters more than most people realize and it is routinely confused by patients and healthcare providers alike. “Sciatica” has become such a widespread catch-all term for any pregnancy-related leg or back pain that enormous numbers of women are being advised to manage a condition they do not actually have. True sciatica caused by irritation or compression of the sciatic nerve is genuinely rare during pregnancy. Research consistently shows that more than 95% of pregnancy-related back and leg pain originates from the SI joint, not from the nervous system.
Why does this matter? Because the two conditions respond to different treatments. Addressing them the wrong way does not just fail to help it can make the wrong condition worse.
| Feature | SI Joint Pain | True Sciatica |
| Where pain lives | Lower back dimple, buttock, upper thigh typically one side | Lower back, travels through the calf, ankle, sometimes into the toes |
| Does it cross the knee? | Rarely usually stays above the knee | Almost always extends below the knee |
| Quality of pain | Sharp, stabbing, achy localized and position-dependent | Burning, electric, shooting follows the nerve pathway continuously |
| Worst triggered by | Single-leg activities: rolling in bed, exiting car, dressing while standing | Bending forward, prolonged sitting, coughing, sneezing |
| Root cause | Joint instability too much or uneven movement in the SI joint | Nerve root compression in the lower spine from a disc or other structure |
| Frequency in pregnancy | Very common affects up to 50% of pregnant women | Quite rare frequently mislabeled and mismanaged |
| Does position change help? | Yes certain positions provide clear, predictable relief | Less so pain can persist regardless of position |
A Simple Self-Check
Point to exactly where your pain is centered. If your finger lands on that dimple above your buttock on one side and the pain does not consistently travel past your knee, the SI joint is almost certainly involved. A pelvic health physical therapist can confirm this clearly in a single assessment and help you avoid weeks of treating the wrong problem.
Eight Effective Ways to Find Relief
1. Pelvic Health Physical Therapy The Gold Standard
Nothing else addresses the root cause of SI joint pain as thoroughly as working with a pelvic health physical therapist. They will assess your specific posture, muscle imbalances, joint behavior, and movement patterns, then build a plan around your body at its current stage of pregnancy. A critical insight from experienced clinicians: the core driver of SI joint pain in pregnancy is almost always muscle weakness rather than the hormone relaxin itself. Strengthening the right muscles particularly the glutes and inner thighs is what creates lasting change. Many women who have been in pain for months feel dramatically better within a few focused sessions.
2. A Maternity SI Belt Temporary Scaffolding for Your Pelvis
An SI belt wraps firmly around the hips and pelvis, providing the external compression that your loosened ligaments currently cannot. Think of it as training wheels for your pelvis during a period when its natural support system is compromised. It works best during activity walking, standing at the kitchen counter, running errands and should generally be removed during rest. It will not resolve the underlying weakness, but it can reduce pain enough to keep you moving while you work on strengthening. Most physical therapists suggest wearing it for two to three weeks initially and then reassessing.
3. Cold for Flares, Heat for Stiffness Used Separately
Cold and heat treat different problems. A cold pack held against the SI joint area for 15 minutes reduces inflammation and numbs sharp pain during an acute flare. Heat via a warm pack, warm shower, or a warm bath relaxes the tight surrounding muscles that cause stiffness, particularly in the morning. Using cold during flares and warmth before movement gives many women the best of both approaches. Always place a cloth between your skin and the pack, and always check with your doctor before using heat therapy during pregnancy.
4. A Birthing Ball Better Posture With No Effort
Sitting on a birthing ball naturally encourages your pelvis to find a more neutral, balanced position the same position that physical therapists spend sessions trying to teach. Gentle circular or side-to-side rocking on the ball also decompresses the SI joint and keeps the surrounding muscles gently engaged. Women with significant third-trimester SI pain often find a birthing ball far more comfortable than any standard chair or sofa. As a bonus, it doubles as excellent preparation for labor comfort positions.
5. Supportive Footwear A Change You Can Make Today
With every step, forces travel up through your feet, ankles, knees, and directly into your pelvis. The shoes you wear either absorb those forces or amplify them before they arrive. Unsupportive footwear worn-out sneakers, flip-flops, flat ballet shoes sends the full impact straight to your SI joint. Shoes with cushioned soles, firm arch support, and a low heel lift dampen those forces significantly. Switching shoes is one of the fastest, lowest-effort changes you can make, and many women notice a difference within the first day.
6. Targeted Muscle Strengthening
The exercises covered in detail in the next section build the specific muscles that directly support and stabilize your SI joint primarily the gluteus maximus, gluteus medius, and inner thigh muscles. Building these muscles is the most effective long-term treatment available, because it addresses what relaxin cannot fix on its own: the muscular support system your pelvis needs to function without pain.
7. Movement Breaks Every 30 to 40 Minutes
Remaining in any single position for too long whether seated at a desk, standing at a counter, or lying on the couch allows the muscles around your SI joint to stiffen progressively. Setting a quiet alarm every 30 to 40 minutes to change position, walk briefly around the room, or perform a gentle stretch keeps blood flowing to the joint, maintains muscle warmth, and prevents the accumulating stiffness that makes late-day pain so much worse than morning pain for most women.
8. Swimming and Water Aerobics
Water removes the effect of gravity. Submerged to shoulder height, your effective body weight drops by roughly 90%, which means you can walk, move your legs, stretch, and exercise your pelvis without the joint loading that makes land-based movement painful. Swimming and water aerobics are consistently cited by pelvic health specialists as among the safest and most effective forms of exercise for pregnant women with SI joint pain especially from the second trimester onward when pain often intensifies on land.
Safe Home Exercises for SI Joint Pain During Pregnancy
Please confirm any new exercise program with your OB-GYN or midwife before starting. Stop immediately if an exercise causes or worsens your pain.
The governing principle for exercising safely with SI joint pain is simple: keep both legs symmetrically loaded. Both feet should stay on the ground, and both sides of your body should be working equally throughout each movement. This single rule eliminates the asymmetric pelvic forces that cause most exercise-related flares.
1: Pelvic Tilts Your Daily Non-Negotiable
Lie on your back with knees bent and feet flat on the floor, arms relaxed at your sides. Breathe in gently, then on the exhale draw your lower belly inward and flatten your lower back against the floor by tilting your pelvis slightly backward. Hold for four to five seconds, breathing normally, then slowly release back to neutral. Perform 12 to 15 repetitions. This activates the deep core muscles that form the first layer of pelvic support muscles that weaken significantly during pregnancy. Done twice daily, pelvic tilts are the single most foundational movement for managing SI joint pain.
2: Glute Bridges Building Your Joint’s Primary Defender
Lie on your back, knees bent, feet hip-width apart and flat on the floor. Press both feet evenly into the ground and squeeze your glutes firmly as you slowly lift your hips off the floor until your body forms a straight diagonal line from your knees to your shoulders. Hold for two to three seconds at the top, feeling the glute contraction, then lower slowly under control. Perform 10 to 12 repetitions. The gluteus maximus is the largest muscle surrounding the SI joint and its primary dynamic stabilizer. Strengthening it consistently reduces joint stress during all the movements that normally trigger pain. Keep your feet parallel and your knees pointing directly forward throughout.
3: Clamshells Targeting the Glute Medius Specifically
Lie on your side with hips stacked directly above each other, knees bent to roughly 45 degrees, and feet lightly together. Keeping your feet touching, slowly rotate your top knee upward toward the ceiling the motion resembles a clamshell opening. Hold for two seconds at the top, then lower with control. Perform 12 to 15 repetitions on each side. The glute medius is a smaller but critically important muscle that stabilizes the pelvis specifically during walking and single-leg activities exactly the movements that most commonly trigger SI joint pain. Consistent clamshell work can produce noticeable improvement in day-to-day pain within two to three weeks.
4: Seated Resistance Band Hip Press Balanced Stability From Both Sides
Sit upright at the edge of a firm chair with feet flat on the floor and a light resistance band looped around your thighs just above the knees. Maintaining an upright posture, press your knees outward against the band, hold for three seconds, then return slowly to the starting position. Perform 10 to 12 repetitions. This exercise simultaneously works the hip abductors (outer hip muscles) and adductors (inner thigh muscles), building balanced support around the pelvis from both directions. It is gentle enough to do several times a day as a break from prolonged sitting, making it ideal for women who work desk jobs.
5: Wall Squats Lower-Body Strength Without the Risk
Stand with your back against a smooth wall, feet shoulder-width apart and positioned roughly 18 to 24 inches out from the wall. Slowly slide your back down the wall until your thighs are roughly parallel to the floor or as far down as feels comfortable without pain. Hold for 20 to 30 seconds, keeping your weight distributed evenly between both feet. Slide back up. Repeat three to five times. Wall squats are one of the safest lower-body strength exercises during pregnancy because the wall prevents the forward trunk lean that puts asymmetric stress on the pelvis in unassisted squats, while the parallel feet ensure both legs are sharing the load equally.
6: Cat-Cow Mobility and Tension Relief for the Whole Spine
Get onto your hands and knees with wrists directly under your shoulders and knees under your hips. On a slow inhale, let your belly drop gently toward the floor, lift your tailbone slightly, and let your head rise (cow position). On a slow exhale, round your entire spine upward toward the ceiling and tuck your tailbone and chin under (cat position). Move gently and continuously between the two positions for eight to ten breath cycles. Cat-cow keeps the lower back mobile and progressively releases the muscle tension that accumulates in the tissues attaching to the pelvis making it particularly valuable for easing the deep morning stiffness that accompanies SI joint pain in pregnancy.
✅ The One Rule That Changes Everything
Stick to exercises where both feet stay on the ground and both sides of your body share the load equally. Swap lunges for wall squats. Swap running for swimming or cycling. Swap the elliptical for the rowing machine. This one behavior change choosing symmetrical over asymmetric movement is the most effective single adjustment you can make to your exercise routine for managing SI joint pain safely during pregnancy.
Movements and Habits That Keep Making It Worse
Sometimes the most immediate relief comes not from adding something new to your day, but from stopping the things that repeatedly irritate the joint without you even realizing they are doing so.
- Standing on one leg to get dressed. Balancing on one foot while pulling on socks, shoes, or trousers is one of the most reliable ways to trigger an acute SI joint flare. Sit down completely before dressing your lower half every single time.
- Crossing your legs when seated. This immediately creates asymmetric pelvic loading and puts uneven pressure on the SI joint. Sit with both feet flat on the floor and your knees hip-width apart instead it feels unnatural at first but makes a significant difference.
- Swinging one leg out of the car independently. Moving one leg out before the other rotates the pelvis and creates a shearing force directly across the SI joint. Instead, pivot your entire body to face the door first, move both legs out together as a unit, then stand up.
- Taking stairs with large, aggressive strides. Large stair steps exaggerate single-leg loading on each step. Take stairs one at a time with a smaller, more controlled step or ascend sideways during a flare if needed.
- Carrying your bump rested on one hip. This creates a persistent lateral pelvic tilt. Try to keep your weight distributed evenly on both feet when standing and avoid propping your belly on one hip as a comfortable rest position.
- Running, lunges, or the elliptical machine. All three create significant asymmetric loading of the pelvis. Replace them with swimming, cycling, walking at a comfortable pace, or the rowing machine during pregnancy.
- Deep, low, or very soft seating. Chairs or sofas that allow your knees to rise above your hip level tip the pelvis into a position that strains the SI joint. Sit in chairs that keep your knees level with or slightly below your hips, and use a lumbar pillow for support.
- Pushing objects with one foot. Sliding a bag, box, or piece of furniture across the floor with your foot places a single-leg rotational force directly through the SI joint a surprisingly common trigger that most women never connect to their pain.
The Best Sleeping Positions for SI Joint Pain During Pregnancy

Nighttime is often when SI joint pain reaches its most uncomfortable. Hours of lying still in a poor position cause progressive stiffening, and any movement rolling over, getting up can produce a jolt of pain that fully wakes you. Getting your sleep setup right is one of the highest-return investments you can make in your daily comfort.
Side Sleeping With Two Pillows
Sleep on your side with one pillow between your knees AND a second between your ankles. This complete stacking arrangement keeps your hips, knees, and feet all aligned preventing the pelvis from rotating and pulling on the SI joint throughout the night. Both knees should remain gently bent and at the same height.
Belly Support Pillow While Side Sleeping
Tucking a thin pillow or folded blanket under your belly from the front relieves the downward pull your growing bump creates on your lower back and pelvis during side sleeping. Combined with the knee and ankle pillows, this three-point support system is the most complete setup for SI joint comfort during pregnancy.
Full Pregnancy Pillow
A full-length C-shaped or U-shaped pregnancy pillow supports your belly, back, and hips simultaneously. For women with significant SI joint pain, these often feel transformative. Choose one that keeps your knees stacked not with the top knee dropping forward for maximum pelvic alignment.
Side Sleeping With Only One Pillow
Using a pillow between your knees but nothing between your ankles allows your lower foot to drop forward, which subtly rotates the pelvis and creates cumulative overnight stress on the SI joint. The ankle pillow is not optional it completes the alignment chain from hip to foot.
✕ Avoid Back Sleeping After 20 Weeks
After 20 weeks, lying flat on your back is not recommended because it can compress a major blood vessel. It also removes pelvic support and increases SI joint pressure. If you wake up on your back, simply roll to your side calmly do not panic about having shifted there.
✕ Avoid Stomach Sleeping
Physically impractical from the second trimester onward, stomach sleeping also forces an exaggerated arch in the lower back that places significant sustained strain on the SI joint and surrounding tissues.
The Log Roll Technique Getting Out of Bed Without Pain
Getting out of bed the wrong way is responsible for a large proportion of early-morning SI joint flares. The instinctive method twisting your upper body while your legs stay behind, or doing a sitting-up motion from flat on your back creates a shearing force directly across the SI joint. The log roll eliminates this completely. Here is the technique: when you are ready to get up, keep your entire body shoulders, hips, and knees pointing in the same direction and roll as one rigid unit onto your side. Do not allow your upper shoulder to twist forward ahead of your hips. Once you are fully on your side with knees bent near the edge of the mattress, use your arms to push yourself to a seated position. Pause for a moment at the edge of the bed, then stand. Practiced consistently, this technique can eliminate the sharp morning jolt almost entirely within a few days.
Smart Daily Habits That Reduce SI Joint Strain
Beyond exercise and sleep, the way you move through an ordinary day has a compounding effect on your SI joint. These adjustments require no equipment and minimal time only awareness.
- Stand with equal weight on both feet. Notice how often you shift your weight to one side when waiting, cooking, or talking. Try consciously distributing your weight evenly and observe how much less strain reaches your pelvis.
- Sit with knees parallel and feet flat on the floor. This seated position is dramatically less stressful on the SI joint than sitting with crossed legs or with one knee raised. It takes two to three days to feel natural.
- Move like a mermaid. When turning, getting into bed, or pivoting in any direction, move your lower body as one unit knees together, hips and legs moving simultaneously rather than letting your upper body rotate away from your pelvis independently.
- Place a lumbar pillow behind your lower back when sitting. A small rolled towel or dedicated lumbar support maintains the natural curve of your lower back and reduces the downstream mechanical stress that reaches your pelvis during prolonged sitting.
- Take a short walk before bed. Ten to fifteen minutes of gentle evening walking improves circulation around the joint, warms the surrounding muscles, and can make nighttime positioning meaningfully more comfortable by reducing pre-sleep stiffness.
- Carry bags symmetrically. Grocery bags, handbags, and shoulder loads on one side create lateral pelvic tilt that accumulates over the course of a day. Divide weight between both hands, or use a backpack to distribute the load evenly across your spine.
- Rearrange frequently used items to be directly in front of you. Reaching across your body or to one side while holding weight a drawer to the left, a shelf to the right creates the rotational pelvic loading that quietly irritates the SI joint throughout the workday.
When to Seek Professional Help
See a Healthcare Provider Promptly If You Experience:
- Pain severe enough that walking, sleeping, or basic daily activities are no longer manageable
- Numbness, tingling, or weakness traveling into your lower leg or foot particularly below the knee
- Pain that began immediately after a fall, a slip, or any physical impact
- Significant pain on both sides of your pelvis simultaneously, which may indicate pubic symphysis dysfunction a related but distinct condition requiring specific management
- Pain accompanied by fever, burning during urination, or any symptoms suggesting infection or other medical cause
- Pain that is worsening rather than improving after two to three weeks of consistent home management
- Any pain that worries you your maternal instincts are reliable, and it is always better to get checked than to wait
One point that deserves to be said directly and clearly: you do not have to wait until after your baby is born to seek help. There is a persistent and harmful myth in pregnancy culture that pain during pregnancy is simply part of the experience and will resolve itself after delivery. The clinical evidence does not support this. Women who actively treat SI joint pain during pregnancy through physical therapy, targeted exercise, and movement modification have significantly better outcomes both during the pregnancy itself and in the months following birth. Women who wait tend to carry the pain forward, sometimes for years, without understanding why it has not resolved.
What Happens to SI Joint Pain After You Give Birth?

Here is the honest picture, without false reassurance. For roughly 80% of women, SI joint pain improves meaningfully within four months of delivery as relaxin levels drop and ligament tension gradually returns to normal. For the remaining 20%, pain persists sometimes for one to three years particularly in women who experienced early-onset pain, prolonged or complicated labor, and in women who breastfeed.
Breastfeeding keeps relaxin circulating at elevated levels for as long as you nurse, which means your ligaments may not fully restabilize until after weaning. This does not mean you should not breastfeed it simply means that if you are postpartum and still experiencing SI joint pain while nursing, this hormonal factor is part of why, and your recovery timeline should be discussed with a physical therapist who understands it.
The postpartum period also introduces new mechanical demands that can sustain SI joint stress long after delivery: repetitive bending to lift your baby, feeding positions that round and compress the lower back, carrying a heavy car seat on one arm, and spending extended hours sitting without adequate back support. A pelvic health physical therapist can guide you through rebuilding strength and returning to normal movement safely and progressively during this period. Every exercise in this guide continues to be relevant and helpful during postpartum recovery.
The most important takeaway: start working on this now, during pregnancy. Building muscle strength and developing better movement habits before your baby arrives makes postpartum recovery significantly faster, and reduces the chance of carrying this pain into the first year of parenthood.
Frequently Asked Questions
How early in pregnancy can SI joint pain start?
SI joint pain can begin as early as the first trimester because relaxin starts rising shortly after conception. Most women notice it becoming significant between weeks 18 and 24 as the baby grows and physical demands on the pelvis increase. Pain that begins before 20 weeks is worth mentioning to your healthcare provider, as early-onset symptoms are associated with a more persistent course throughout pregnancy and postpartum.
Does SI joint pain during pregnancy go away after delivery?
For roughly 80% of women, pain eases meaningfully within four months of giving birth as hormone levels normalize. About 20% experience ongoing pain for up to three years postpartum particularly those who did not address it during pregnancy. Women who breastfeed may take longer to recover because relaxin remains elevated during nursing. Treating SI joint pain actively during pregnancy significantly improves outcomes after birth.
How is SI joint pain different from sciatica during pregnancy?
SI joint pain sits in the lower back dimple, buttock, and upper thigh typically one side and is triggered by single-leg movements. True sciatica involves nerve compression producing burning or electric pain that travels past the knee into the calf, ankle, or foot. Research indicates that over 95% of pregnancy-related back and leg pain originates from the SI joint, not the sciatic nerve despite sciatica being the term most commonly used to describe it.
What is the safest way to sleep with SI joint pain during pregnancy?
Sleep on your side with a pillow between your knees AND a second pillow between your ankles. This dual-pillow arrangement keeps your entire lower body aligned from hip to foot and prevents your pelvis from rotating overnight the primary cause of that sharp pain that hits the moment you move in the morning. Adding a thin pillow under your belly from the front provides additional support as your bump grows.
Which exercises are safe for SI joint pain during pregnancy?
Safe options include glute bridges, pelvic tilts, clamshells, seated resistance band hip presses, wall squats, and cat-cow stretches. The core principle is symmetry: both legs should be working equally throughout every movement. Avoid lunges, running, single-leg exercises, and the elliptical machine, which load one side of the pelvis disproportionately. Always confirm with your OB-GYN or midwife before starting any new exercise during pregnancy.
Is walking safe with SI joint pain during pregnancy?
For most women, yes. Gentle walking keeps surrounding muscles warm and active, which supports the joint. However, if walking consistently causes limping, worsens your pain during the activity, or leaves you significantly sore for hours afterward, shorten your distance, wear properly supportive shoes, and consider adding a maternity SI belt during walks. If these adjustments do not help, consult a pelvic health physical therapist before continuing.
Can SI joint pain affect labor and delivery?
SI joint pain does not directly endanger your baby. However, significant pelvic instability can make labor positions more uncomfortable and may influence how your body moves through the birthing process. A pelvic health physical therapist who specializes in pregnancy can advise you on specific birth positions and movement strategies designed to minimize SI joint stress during labor a conversation well worth having before your due date.
Can I reduce the risk of SI joint pain in a future pregnancy?
You cannot guarantee prevention, but you can lower your risk considerably. Entering pregnancy with strong glutes, a stable core, and good movement awareness gives your SI joints significantly better protection against the hormonal and mechanical changes of pregnancy. If you have experienced SI joint pain before, beginning work with a pelvic health physical therapist either before conception or in very early pregnancy gives you the strongest possible foundatio
Conclusion:
SI joint pain is one of the most common discomforts in pregnancy and one of the most treatable. Common does not mean inevitable, and it absolutely does not mean you have to push through it for nine months.
Start with the habits that cost nothing and take no equipment: sit down every time you get dressed, stop crossing your legs, sleep with pillows between your knees and ankles, and move your entire lower body as one unit whenever you turn or pivot. Layer in the strengthening exercises as your body allows. And if the pain is affecting your sleep, your movement, or your ability to enjoy this time, reach out to a pelvic health physical therapist.
Do not wait until after your baby arrives. The earlier you start, the better you will feel during pregnancy and in every month that follows.
Medical Disclaimer:
This article is written for general informational and educational purposes only. It does not constitute medical advice, diagnosis, or treatment. Every pregnancy is different. Always consult your OB-GYN, certified midwife, or a licensed pelvic health physical therapist before starting any new exercise program or treatment during pregnancy especially if you are experiencing severe, worsening, or unusual pain.